Eczema Treatment
Have you ever had rough patches of skin? The kind which are looking inflamed, are itchy and also rough? This may be eczema and you may need to get eczema treatment.
Eczema is actually a very common skin condition. It is when your skin is feeling super itchy and is also red.
The condition can take on any time but usually it is taking place at an early age. Like during infancy or even early childhood.
If you don’t get eczema treatment, the condition will only get worse if you don’t get it looked at right away.
When we talk about eczema there are actually different kinds.
When a doctor looks at the eczema you have, the doctor will treat it in a way to make sure the rash you are developing is in complete control.
While this is not a kind of harmful condition, it is something that can progress uncontrollably if you don’t get eczema treatment on time.
In this article I will be sharing details on how you can identify it, the causes and ways to resolve it.
So let’s begin:
What Causes Eczema?

So this is where the doctors are also completely perplexed.
They are also not clear completely on what is eczema.
Some suggest that it takes over due to having skin which is having heavy exposure to external irritants.
These will cause your immune system to overreact.
And when it does, you will notice there are many reasons as to why it will flare up.
Also if a person is having eczema, it is possible that they are not making a lot of protein.
This protein is known as filaggrin.
It is actually an important protein. Because it helps in keeping your skin feeling moisturized and being healthy.
But having it in excess will cause you potential harm in the long run.
Now let’s look into some of the leading causes of eczema.
Why Eczema Happens?
There are plenty of things which can trigger eczema in a body. It is not common for you to have it.
Which means your body is getting exposure to certain conditions which is causing it to react in some way.
There are so many factors which contribute to how you look.
I will be sharing some of the leading potential irritants. These will be causing you to have an allergic reaction.
So what is triggering eczema in your body:
- You are having major exposure to dry air. This means whether it is extreme heat or cold, it is going to be causing you to suffer from eczema.
- There are also certain kinds of soaps, shampoos, even bubble baths which can trigger eczema
- This includes body wash as well as facial cleansers. Make sure you have a good handle on them.
- Otherwise your skin will be suffering completely.
- There are candles which have a lot of fragrance in them. Make sure you avoid their use.
- Certain fabrics like wool and polyester also make your skin irritating.
- Also if you make use of metals, they too can make use skin look extremely hurt and red.
- People who are using natural liquids, like fruit and vegetables will be having this condition. It is quite possible.
- There is also a kind of antibacterial which we find in things like hand and baby wipes. This is extremely harmful and can make your skin extremely irritated and painful.
- Among other causes, having emotional stress can also lead to this condition. There are different symptoms that can take over in this regard. It can flare-up for no reason and make you extremely stressed and irritated.
Now let’s look into the symptoms you may be having.
Symptoms of Eczema

It is essential that you are able to identify the signs to know what is eczema.
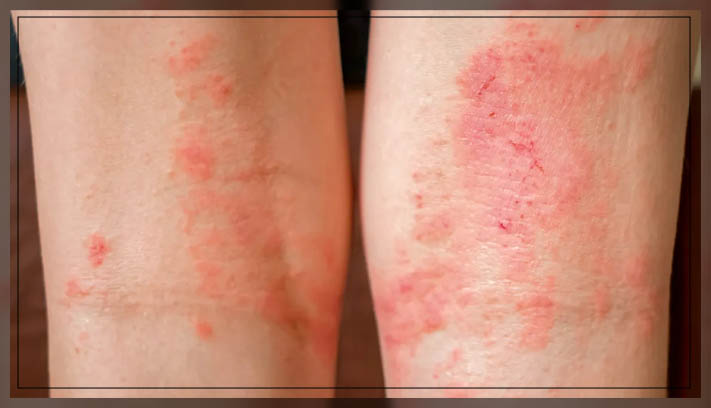
One thing and the first thing you will notice is that it is essentially making your skin appear a lighter red, making it extremely light.
Also you will notice that it also has plenty of dark brown and it is light purple in color.
The major signs to look out for:
- They will be itchy. This is little but can quickly escalate where you cannot stop the itching at all.
- Having dry and sensitive skin is a leading cause for you to get this condition. It can become extremely sensitive and will make you feel itchy all the way.
- Inflammation and discoloration is common in this condition. This is a major suggestion that something is wrong
- Rough and leathery skin can happen as well. It can only worsen with time.
- You will notice oozing and a crusting feeling which continues for long.
- There will be some areas of swelling. It is going to spread if you don’t combat it.
These are some of the most common symptoms. You have to make sure you are getting a complete knowledge on how it will be leading several issues.
But the best thing to do is that you have to consult a healthcare provider.
They will be ensuring you get a complete health makeover. There are some of the major signs that suggest that you will be needing a healthy lookout.
Eczema Treatment

Now we come to the most important element of all.
Is there an effective cure for eczema?
Well while we cannot say you can cure it completely. The fact is you can make sure you are getting effective treatment.
It all depends on your age and how severe the condition is.
There are several treatments in this regard that give results.
Among them are moisturizing creams as well as over the counter treatments.
You can also get injectable biologics.
They work really well and allow you to have natural as well as alternative treatments.
This includes having bleach baths, meditation as well as acupuncture.
But when deciding on what kind of treatment to go for, you have to look at your own symptoms. Things to watch out for:
- You should be knowing your own triggers. Looking at the kind of exposure you get enables you to get a complete overlook.
- Implementing a daily bathing and moisturizing routine helps. It helps in big ways to clear off all the buildup of skin infection.
- But for that as well, you have to make sure you are adapting all the essentials needed to make your skin look bright and beaming,
- Some doctors also suggest making use of OTC creams.
- Drinking plenty of water helps
- These as well as prescription medication can serve you in the long run. Allowing you to look exquisite and vibrant as ever.
But one thing to know is that symptoms can actually vary from one person to another. Some may be suffering from very severe symptoms.
Others may not.
You have to get a good handle on what are you going through.
This allows you to handle the condition in a certain manner, ensuring you see ample results when doing so.
In many cases, the eczema will get better or it will completely go away as the child gets bigger.
However in some rare conditions, it might even progress into adulthood. To the point where any kind of medication will not be showing major results in curing your condition anymore.
Also it is quite possible that adults may also suffer from this condition.
They can also develop severe conditions which will only worsen as time progresses.
It is quite possible for you to suffer from this for a while and even if you didn’t have eczema has a child, it is quite possible you may suffer from it.
Homecare Matters
When talking about eczema, one thing to know is that you can actually adapt certain treatments right at home which will allow you to control its spread.
Some of the essentials ways in which you can combat how it impacts your skin include:
- Take lukewarm waters
- You should aim to apply moisturizers as soon as you take bath. This will allow you to lock in the moisture effectively.
- Make it a habit to moisturize everyday.
- Wearing cotton and soft fabrics is a good way of combating it. Doing so does not irritate your skin. Ensuring you are locking the moisture.
- Whether its hot or cold, you should be using a humidifier often.
- This keeps the air moist for long hours.
- Air drying and gently patting it is an effective way to lock in the moisture and keep it dry.
- You should be also taking some extra precautions which helps in the prevention of eczema.
- Adapting and taking small measures will only help to strengthen you and allow you to get the most from your skincare.
Conclusion
Having your skin looking fresh is not always an easy task. Especially if you are suffering from something like eczema.
This is a skin condition which can make your skin look flaky. It also causes it to be red and itchy.
All these factors suggest you have a condition which needs treatment.
Eczema treatment can be of different kinds. It all comes down to knowing what works for you.
You have to break down and look at the ways in which you can ensure it is going to be making a difference to how you get treatment.
While there is no cure for eczema, the fact is you can get a complete treatment when you have apply such kind of ways to get a handle on it.

